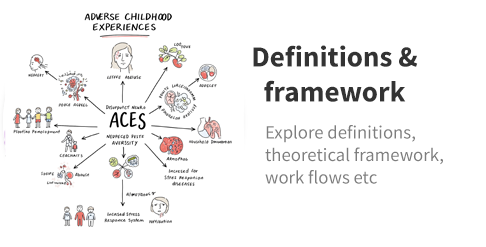
About ACEs in EHRs
The ACEsinEHRs platform provides validated domains, indicators, and code lists to identify adverse childhood experiences (ACEs) in routinely collected non-identifiable electronic healthcare records of parents and children before and after birth.
Adverse childhood experiences
Adverse childhood experiences (ACEs) are potentially traumatic, violent, or neglectful events in childhood that can have a profound impact on a child’s health and development (1).
Examples of recorded ACEs include child maltreatment (e.g., child protection interventions), exposure to domestic violence, and growing up with a parent experiencing mental health or substance use problems (often referred to as the 'trio of vulnerabilities') (2).
ACEs in EHRs
Electronic health records (EHRs) contain a wealth of routinely collected information about patients, including their medical, medication, and social histories. ACEsinEHRs is a platform that provides clinically relevant and validated indicators to identify these experiences within EHRs.
These indicators are based on several rigorous studies (3, 4, 5) and inspired by the landmark Adverse Childhood Experiences (ACE) Study, which established that exposure to ACEs is strongly associated with a wide range of adverse health outcomes.
Mission statement and aims
EHRs are routinely collected and readily available. However, there are significant challenges in using them to inform practice and policy. EHRs are often stored across disparate databases, organisations, and coding systems, resulting in a complex web of data requiring specialist management skills. Prior to this platform, there was no validated set of indicators for identifying ACEs in EHRs using both parent and child data.
Our Mission
- To improve the health of families and young people by utilising electronic health records (EHRs) to identify and measure ACEs.
- To advocate for early support and family-centred services for families affected by ACEs.
- To collaborate with researchers, professionals, and policymakers to promote trauma-informed care and public health policies.
- To enhance the methodological standards, accessibility, and utility of data-driven, 'think-family' approaches.
- To continuously develop the ACEsinEHRs platform to improve resources for the wider clinical and research community.
Key Achievements
- Developed common data standards and comprehensive coding systems for tracking ACEs in EHRs.
- Created sophisticated data management tools and resources, making ACE indicators readily accessible and usable for external researchers.
- Pioneered methodologies for reliably linking and studying EHR data across multiple family members.
All platform activity is publicly logged. All code for data management and analysis is shared under open licenses.
We follow WHO's Minsk Declaration and view ACEs through a "life-course" and a "trauma-informed" lens. This approach acknowledges that risk is not static and depends on the interaction of multiple unmeasured promotive, protective, and risk factors throughout generations and people's lives.
Real-World Impact:
From Research to Results
The ACEsinEHRs open-access platform shares essential coding algorithms, tutorials, and theoretical frameworks that have been widely adopted by researchers globally.
Latest Citing Research

The Role of Artificial Intelligence for Intimate Partner Violence Prevention: A Systematic Review
Li et al. - 2026
Intimate partner violence (IPV), encompassing physical, sexual, emotional and economic abuse, remains a pervasive global health concern. Traditional prevention efforts...
Artificial intelligence in applied family research involving families with young children: A scoping review
Lee et al. - 2025
This scoping review systematically examined the applied family science literature involving families raising young children to understand how relevant studies have applied...
Adverse childhood experiences in firstborns and mental health risk and health-care use in siblings: a population-based birth cohort study
Syed et al. - 2025
Adverse childhood experiences (ACEs) often affect multiple children within families, yet studies tend to focus on the health outcomes of individual children...
Applying analytics to sociodemographic disparities in mental health
Baird & Xia - 2025
Mental health services and treatment are unfortunately subject to sociodemographic disparities. To address this issue, recent studies have begun to apply analytics methods...
Machine learning for prediction of childhood mental health problems in social care
Crowley et al. - 2025
Rates of childhood mental health problems are increasing in the UK. Early identification of childhood mental health problems is challenging but critical to children's...
Examining the rollout of the Triple P system parenting program in Manitoba on rates of child maltreatment
Joshi et al. - 2025
Triple P is a multilevel parenting program aimed at promoting children's emotional, social, and behavioural competence and preventing behavioural problems...
Preconception indicators and associations with health outcomes reported in UK routine primary care data: a systematic review
Schoenaker et al. - 2024
Routine primary care data may be a valuable resource for preconception health research and informing provision of preconception care. Aim: To review how primary...
Revisiting the use of adverse childhood experience screening in healthcare settings
Danese et al. - 2024
Adverse childhood experiences (ACEs) are key modifiable risk factors for mental illness. The potential to detect and mitigate ACEs to improve population mental health...
The association between adverse childhood experiences and mental health, behaviour, and educational performance in adolescence
Lam et al. - 2024
Adverse childhood experiences (ACEs) are thought to have negative effects on mental health and well-being in adolescence. The definition of ACEs varies between studies...
Access without borders: a scoping review to identify solutions to creating portable identity, education and health records for refugee children
Ungar & Seymour - 2024
The focus of this scoping review is to identify studies, reports, and other relevant sources from the peer-reviewed and grey literature that reports on refugee children's access...
Advantages of EHRs
ACEs are preventable. However, many are exceptionally difficult to identify during childhood. Most traditional studies rely on adults' retrospective self-reports many years after the event, which are prone to memory biases. This "time gap" means data is collected too late to prevent the immediate harmful effects.
Conversely, EHRs provide prospectively recorded data from hospitals, GPs, and other health systems as events naturally happen during routine care. This information becomes available shortly after a healthcare presentation and poses far less burden on patients than completing complex research surveys.
Crucially, in the UK, mothers' and children's EHRs can be securely linked across services. This unique capability allows researchers to seamlessly measure ACEs before pregnancy, throughout childhood, and intergenerationally.
Limitations of ACEs in EHRs
When utilising this library, it is essential to note:
- There are methodological challenges in accurately linking children’s EHRs to their fathers’ EHRs (a long-standing limitation of anonymised secondary and primary care data). Consequently, current ACE research using EHRs has primarily been based on linked maternal and child data.
- The platform only identifies experiences recorded in semi-structured, coded non-identifiable data. Serious concerns recorded solely in free-text clinical notes will not be captured by these coded indicators.
- The indicators do not represent an exhaustive list of all possible adversities experienced by children.
- Cannot make inferences about an individual. This means that indicators cannot be used to guide individual-level clinical decision-making, including screening, diagnosing, or labelling children or families to be at risk of harm.
- Do not assume children with ACEs will inevitably develop poorer health outcomes. Most children with ACEs do not develop poorer health outcomes and show profound resilience.
- These records do not account for mitigating protective factors and wider systemic contexts.
Team & Contributors
This project was developed by a range of researchers and clinical experts:
1. UCL Great Ormond Street Institute of Child Health, Population, Policy and Practice, Faculty of Population Health Sciences London WC1N 1EH.
2. Oxford Institute of Clinical Psychology Training and Research, University of Oxford, Oxford, UK.
3. Institute of Health Informatics and Health Data Research UK, University College London.
4. Bristol Medical School, Bristol Population Health Science Institute Centre for Academic Primary Care, University of Bristol.
5. General Practitioner, NHS.
6. Paediatric Pain Research Group, University College London Great Ormond Street, Institute of Child Health, London WC1N 1EH.
7. Department of Anaesthesia & Pain Medicine, Great Ormond Street Hospital for Children NHS Foundation Trust.
Feedback & Contributions
We are continuously working to make this platform and the ACE indicators easier to access and implement. This website is open source and hosted via Github.
If you would like to contribute or provide feedback, please get in touch at s.syed.16@ucl.ac.uk
Acknowledgements
Study Support: This webpage accompanies a study that uses patients' data collected by the NHS as part of their care #DataSavesLives. We are extremely grateful to the generosity of the patients and their families, along with the participating GP practices and NHS staff, for their ongoing contribution to mental health and family violence research.
The ACEs studies (protocols: 19_162R, 21_000587) were approved by the MHRA (UK) Independent Scientific Advisory Committee, under Section 251 (NHS Social Care Act 2006). The studies were carried out as part of the CALIBER© resource. CALIBER, led by the UCL Institute of Health Informatics, is a research resource providing validated electronic health record phenotyping algorithms and tools for national structured data sources.
The ACEs studies are based on data from the CPRD obtained under licence from the UK Medicines and Healthcare products Regulatory Agency. The interpretation and conclusions contained in this study are those of the author/s alone. HES, and ONS are under copyright © (2020), re-used with the permission of The Health & Social Care Information Centre. All rights reserved.
The research was supported in part by the NIHR Great Ormond Street Hospital Biomedical Research Centre. This research benefits from and contributes to the NIHR Children and Families Policy Research Unit, but was not commissioned by the National Institute for Health Research (NIHR) Policy Research Programme. The views expressed are those of the author(s) and not necessarily those of the NHS, the National Institute for Health Research, the Department of Health and Social Care or its arm's length bodies, and other Government Departments.